With out pressing reform, the NHS is doomed. That is the grim analysis by Liam Hughes, who spent half a century working for the well being service

Liam Hughes’ new ebook, Bodily Fluids, units out a lifesaving prescription for the NHS (Picture: Courtesy Liam Hughes)
After beginning within the 50s, the BBC drama Name the Midwife has now reached the 70s, the last decade when my profession began. Within the years main as much as my retirement two years in the past, some youthful colleagues affectionately referred to as me a dinosaur with rose-tinted spectacles each time I lamented the passing of the outdated regime.
However given the relentless rise in dissatisfaction amongst sufferers, their kin and well being suppliers, revisiting earlier fashions of care and coaching can spotlight a method ahead for the failing NHS. Morale is dangerously low and the NHS has been stripped of its once-universal esprit de corps. The potential causes are many and there’s no fast repair, however with out surgical procedure our once-favourite establishment will flatline.
Rebuilding the esprit de corps
The medical workforce is much less united than ever earlier than. GPs and hospital medical doctors have little contact, with each teams blaming one another when issues go unsuitable. The identical is true for the connection between residents and consultants. In my first 12 months, I had one notably busy weekend on name. I clerked the admission of 53 sufferers, all of whom had a GP letter or had been mentioned with me or my advisor.
The Monday morning spherical took till the night, after which we had been handled to beer and a curry by the boss. I nonetheless keep in mind a few of the circumstances and discovered extra in a number of days than months as a scholar. I offered a whole lot of sufferers to the crew and obtained priceless suggestions on all my selections. This sense of assist gave me confidence.
Right now, based mostly on my conversations with youthful colleagues, it’s clear that first-year medics have a very completely different expertise. Working a mean of 4 11.5-hour shifts every week, few work for a particular advisor they usually usually spend shifts in numerous departments. Many stay unaware of what occurred to sufferers they assessed, and none reported the dopamine buzz of being given thanks by recovered sufferers.
One advised me that every one sufferers admitted to their ward had been designated not for resuscitation. Nobody I spoke to had been for an off-duty meal or drink with any co-workers and definitely not a advisor, and lots of reported feeling remoted and unsupported.
This can’t occur with out common master-and-pupil suggestions on hundreds of circumstances which present resident medical doctors are lacking out on. Whereas I discovered it arduous as a scholar to recollect the branches of the brachial plexus or the phases of the Krebs cycle, recalling the histories and check outcomes of sufferers got here simply to me.
It’s a facility I by no means misplaced. It is because that data had actual consequence and, ingrained by my early bosses, it emphasised the significance of taking proprietorial accountability for sufferers underneath your care. This not often occurs in 2026. Quite, sufferers are sometimes underneath a division with consultants working a rota, generally altering each day. Medical doctors additionally rotate, so continuity is misplaced. That is harmful for sufferers and a catastrophe for coaching.
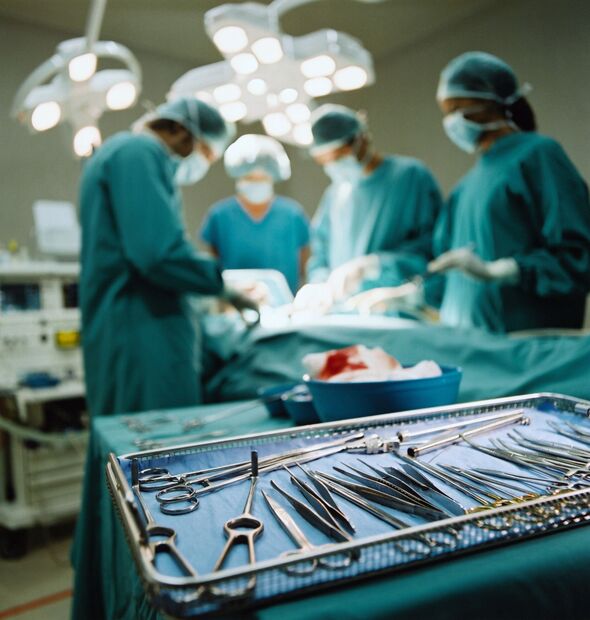
Shift work in hospitals radically will increase the variety of assessments and investigations sufferers bear (Picture: Getty)
Shift work causes pointless investigations
Working in shifts will increase the variety of investigations sufferers bear. This primarily applies to acute admissions. Medical doctors will solely have a 50% probability of seeing the affected person once more. Arranging an imaging check, for instance, delays the necessity to instigate therapy. That call might be deferred to the next crew with out the danger of being accused of leaping in with a selected therapy. At senior stage, ego will generally additionally trigger one advisor to rearrange esoteric assessments to impress the handover crew. Few will imagine this occurs, however most senior medical doctors understand it to be true.
We’d like ‘corporations’, not shifts
Restoring a “agency” somewhat than a “shift” mannequin of care would profit all however making the change shall be nigh-on not possible. The tiredness argument shall be raised and the recognized documented dangers of fixed affected person handovers shall be dismissed. Taking care of sufferers over a 24-hour interval might be secure if there are brief breaks. It’s extra akin to crusing solo within the Southern Ocean than driving a petroleum tanker down a motorway (essentially the most often-quoted instance within the argument towards lengthy hours).
The latter requires absolute unbroken focus with out distraction; the previous, as round-the-world sailor Alex Thomson has defined, requires brief durations of relaxation as and when potential, coupled with laser-like focus when on deck.
A “agency” system would additionally make a person advisor answerable for every affected person. Senior cowl ought to rotate weekly not each day, so sufferers and their kin have continuity. Sufferers beforehand admitted underneath one advisor ought to be handed again if readmitted. Every day the advisor may see the brand new admissions with the in a single day first-year physician by conducting a 6am spherical which permits the resident to go off obligation on time.
First 12 months medical doctors ought to take care of particular person sufferers:Permitting first-year medical doctors to take care of sufferers in such a rota with the suitable assist from an on-site center grade and advisor accessible for calls would improve their expertise. Medical doctors in acute specialities shouldn’t be working in shifts. This isn’t merely higher care however politically important. As soon as medical doctors grew to become simply one other shift-based supplier of care, they misplaced political energy and governments have exploited this.
My recommendation to anybody admitted could be to ask the identify and phone particulars of the advisor who will oversee their care and the occasions when the admitting resident physician shall be on obligation. I’d additionally add the identify of the senior nurse overseeing my care. These aren’t unreasonable requests, however many NHS inpatients gained’t know who oversees their care.
Hughes as a younger NHS physician nearer the start of his lengthy profession (Picture: Courtesy Liam Hughes)
Man the barricades
Hospital beds are a scarce useful resource. At present, they’re provided to many individuals who don’t require one and others who could be higher cared for elsewhere.
The shameful underfunding of major care has resulted in sufferers who’re determined to see a physician, turning to their native hospital. The GP service will take years to restore however, within the meantime, hospitals ought to redeploy their employees to satisfy this large inflow. A examine I carried out 10 years in the past would possibly provide a option to scale back admissions. Senior medical doctors in command of entrance door areas are extremely skilled, however they’re generalists with good understanding of a really big selection of situations.
To help their choice making, particularly relating to whether or not the affected person must be admitted, quite a few protocols have been developed. The rules relating to some signs are risk-averse, which leads to many admissions that become pointless after later overview by a specialist.
One such symptom is chest ache. Most individuals aren’t at fast danger, however each the sufferer and physician fear as chest ache can point out a life-threatening trigger in a small proportion of circumstances. Proving that somebody’s chest ache doesn’t have a life-threatening trigger is way extra difficult than detecting those that do have one. Once I reviewed this cohort of sufferers, round 70% didn’t require admission.
Well being information, recommendation and signs to be careful for Subscribe Invalid e-mail
We use your sign-up to offer content material in methods you’ve got consented to and to enhance our understanding of you. This will likely embody adverts from us and third events based mostly on our understanding. You’ll be able to unsubscribe at any time. Learn our Privateness Coverage
Everyone knows the frustration brought about by the point it takes from attending A&E to getting a choice. Deploying the on-call advisor for each speciality would streamline therapy and the important choice about whether or not to confess or not. Even these whose admission depends upon a check consequence would profit because the system wouldn’t be overwhelmed by the over-investigation of low-risk sufferers by much less skilled employees.
- Liam Hughes spent practically 5 many years on the NHS frontline, in the end as a senior heart specialist earlier than retiring two years in the past. His new ebook, Bodily Fluids, lays out a radical new prescription to avoid wasting the NHS

Bodily Fluids by Liam Hughes recounts the writer’s five-decade NHS profession (Picture: Eye Books)


















Leave a Reply